Treponema pallidum morphology and culture
Belongs to the genus Treponema pallidum, family Spirochaetaceae. Are more pathogenic subspecies pallidum ssp. endemicum (disease Bejel), ssp. pertenue (disease yaws) and ssp. However carateum (disease Pinta), these species are found only outside Europe, but may cross-react in serological testing. It is gram-negative spiral bacteria with poor dyeability that survive outside the body for only a short time longer, however, as in blood. A culture is not currently possible, but cultivation in rabbit testes.
Treponema pallidum epidemiology
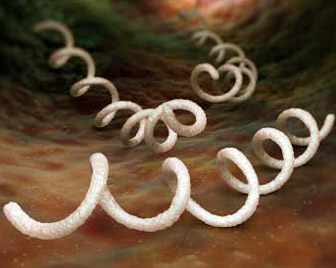
Treponema pallidum is spread worldwide, the first description of an outbreak in Europe in 1494 at the siege of Naples. A very good description of the chain of infection is found in the 1759 published novel Candide by Voltaire. The incidence in Germany in 2008 to 3.9 Fällen/100.000 inhabitants,. Proportion of women dropped to 7%. In some cities (eg Berlin, Hamburg, Munich) outbreaks were registered, only men were affected with a high rate of reinfection. There is a close connection between positive syphilis serology and HIV seroconversion. The number of congenital diseases is very low with one to seven cases.
Pathogenesis, disease (syphilis / syphilis)
The pathogens penetrate the genital (or other) membrane and disseminate via the lymphatic route and via the bloodstream throughout the body, including the CNS. A transfer is both transplacentally as possible via blood transfusions. Clinical symptoms, there are only about 50% of infections, and the course of the disease is divided into three clinical stages: the primary stage (syphilis I) with occurrence of a primary lesion (ulcus durum or hard chancre) with edges incubation painless, sharply defined, not undermined (9) -14 to 24 - (90) days. The primary lesion is localized as on the genitals, mouth, anus, and at other contact points. These lesions are highly infectious! The regional lymph nodes are swollen. The healing of the primary complex (ulcus durum plus swollen lymph nodes) occurs after four to six weeks.
Beginning of the secondary stage (secondary syphilis, infectious) to (4) -6 to 10 - (12) weeks with rashes (usually derived stresses) and Enanthemen with occurrence of angina stomatitis, painless enlargement of the lymph nodes and in the mucous membranes of the mouth, anus and vaginal moist papules (condylomata lata) with numerous treponemes. Modesty can be a specifica areolaris alopecia, the hair and beard area contains raspberry papillomas similar to cauliflower. On lateral neck depigmentation are ("collar of Venus") and on the plantar surfaces of the hands and soles of the feet excessive callus formation (clavi syphilitici) was observed. In stage II, eye involvement as a possible form of a bilateral anterior uveitis. After about two years, the skin symptoms subside. After some years of latency (syphilis latens seropositiva), the tertiary stage (syphilis III) occur with the participation of the aorta (aortitis Luetica, aneurysms), myocarditis, and with ulcerating granulomatous changes in all organs (gums, painless tumors of elastic consistency with central liquefaction) and tuberous lesions. In the late stage it comes to the neurosyphilis (CNS) with tabes dorsalis (degeneration of the posterior columns of the spinal cord paraesthesia, pain in the lower abdomen and legs, about 20 years after initial infection), syphilitic meningitis with paraesthesia and paraplegia, hemiplegia and hemiparesis, aphasia and seizures. After 15-20 years, a progressive paralysis (Argyll Robertson phenomenon with impaired light response with preserved convergence reaction) developed in death after about four to five years. In the course of hematogenous dissemination also an infestation of the liver is possible, the result is a hepatitis with some transition to cirrhosis. Gumma also manifest itself in the liver.
Prevention, treatment, mandatory reporting
A major significance of the exposure prophylaxis and prevention through education of sick people as well as contact persons. See www.ndrugs.com for medications. (Switzerland procaine penicillin STREULI,) or procaine penicillin used, the therapy is primarily penicillin [relatively poor Liquorgängigkeit Benzylpenicillin benzathine (TARDOCILLIN others)]. Alternatives are ceftriaxone (Rocephin others), doxycycline (DOXYHEXAL etc.) or azithromycin (ZITHROMAX others), being reported on resistance to azithromycin. Prevention of Jarisch-Herxheimer reaction can prednisolone (Decortin H, etc.) 24h prior to treatment over three days will be given. A non-nominative mandatory reporting of acute or previously unrecognized active disease is according to § 7 IfSG.
| Name | Dosage | |
| Tetracycline | 250 - 500 mgs | 4 times a day for 5-7 days |
| Gentamicin | Intramuscular, intravenous. 3 mgs / kg /day (max 5 mgs / kg /day) every 6-8 hours | 7 - 10 days |
| Norfloxacin | 400 mgs | twice a day for 7-14 days |
| Spectinomycin | 2 g single dose or as two injections at different sites (total 4 g) | once |
| Ciprofloxacin | 500 mgs | twice a day for 7 - 14 days |
| Erythromycin | 250 - 500 mgs | 4 times a day at least 2 hours before a meal |
| Miramistin | 2-10 ml | For emergency prevention of sexually transmitted diseases: no more than 2 hours from the time of a random sexual encounter after a careful toilet vulva treat them liberally moistened cotton swab, then 1-1.5 ml - intrauretralnogo and women additionally performed vaginal douching 5-10 ml preparation. |
| Azithromycin | 250 - 500 mgs | once a day at least 1 hour before or 2 hours following a meal |
| Benzalkonium chloride | Apply at the rate of 0.2-0.4 g/cm2 wound surface (max 50 gramm a day) | for 14 days. |
|
Pregnancy
With acquisition of the infection during pregnancy, the child in utero (congenital syphilis) ill, a diaplazentarer crossing the treponemes in any stage of pregnancy is possible (70-100% in primary syphilis, 70% in secondary, 40-80% for early latent and 10% for late latent syphilis). There are virtually all infected organs, about 50% of fetuses die off, the remaining postpartum women show different forms of the disease. Approx. 60% of children are asymptomatic at birth. Congenital pneumonia are observed.
Newborn: early form within the first two years of life, especially in the first months of life with skin and mucosal lesions, syphilitic osteochondritis, anemia and hepatosplenomegaly. The late form is usually manifested shortly before puberty with Hutchinson's triad (keratitis, dental deformities, deafness), and neurosyphilis and cardiovascular lesions.
Diagnosis
Routine testing is carried out in pregnant women, blood donors, individuals diagnosed with a sexually transmitted disease, including HIV or people with the risk of acquiring such a disease (eg partner), people with hepatitis B or C, with suspected neurosyphilis (sudden visual or hearing loss, meningitis). Detection of Treponema pallidum succeed in the dark field microscope (non-specific, such as confusion with oral, non-pathogenic spirochetes) or specifically by PCR. The serological detection is primarily about screening tests such as enzyme immunoassay, Treponema pallidum particle agglutination (TPPA ), may repeat one to two weeks after a negative test result. Despite positive findings confirmatory test such as FTA-absorption test (FTA-ABS IgG test), in addition cardiolipin CBR or VDRL test (lipid-Ab) and / or 19s-IgM-FTA-ABS test. An IgM-negative findings includes an active, not requiring treatment of syphilis, nor a negative or a low responding VDRL or cardiolipin CBR. In addition, an immunoblot is necessary. A confirmation must be in a second blood sample. Diagnosis of congenital syphilis: detection of IgM antibodies (immunoblot) or positive PCR findings in the newborn. Titerkontrollen after 1, 2, 3, 6 and 12 months or until a negative result is obtained. Diagnosis of neurosyphilis: Detection of intrathecal antibody synthesis, determination of the function of the blood-CSF barrier by means of albumin quotient and total protein determination.
|